Recent Blog Posts
Study Links Popular Heartburn Medications to an Increased Risk of Dementia
 All medications come with risks, but some have more than others. Unfortunately, the risks are not adequately researched, or worse, properly disclosed to prescribing physicians and patients. The warnings, in many instances, are inadequate. Such instances involving dangerous or defective drugs can wreak havoc on the lives of unsuspecting victims. Case in point: the recent study that revealed popular heartburn medications may carry an elevated risk of dementia.
All medications come with risks, but some have more than others. Unfortunately, the risks are not adequately researched, or worse, properly disclosed to prescribing physicians and patients. The warnings, in many instances, are inadequate. Such instances involving dangerous or defective drugs can wreak havoc on the lives of unsuspecting victims. Case in point: the recent study that revealed popular heartburn medications may carry an elevated risk of dementia.
Proton Pump Inhibitors and Their Uses
Proton pump inhibitors, or PPIs, are a class of drugs used to treat certain gastric conditions, including peptic and stomach ulcers, acid reflux, and gastroesophageal reflux disease (GERD). Available both by prescription and over the counter, they are used by an estimated 15 million Americans. Some who take them claim they are difficult to stop because the condition returns with an increase in severity. But, in light of recent studies, cessation of use may very well be the best course of action, particularly for those who suffer from milder versions of the treated conditions.
Yale Physician Accused of Removing Wrong Body Part and Trying to Cover it Up
 Now considered the third leading cause of death in the United States, preventable medical mistakes are trumped only by cancer and heart disease. Mistakes that cause harm, serious injury, or unnecessary stress are also extremely prevalent. Yet regulations, lawmakers, and even the doctors and hospitals themselves fail to take action or accountability. One woman, who allegedly had the wrong rib removed during a surgery at Yale hospital, had just this sort of an experience when the doctor reportedly tried to cover up his mistake instead of apologizing.
Now considered the third leading cause of death in the United States, preventable medical mistakes are trumped only by cancer and heart disease. Mistakes that cause harm, serious injury, or unnecessary stress are also extremely prevalent. Yet regulations, lawmakers, and even the doctors and hospitals themselves fail to take action or accountability. One woman, who allegedly had the wrong rib removed during a surgery at Yale hospital, had just this sort of an experience when the doctor reportedly tried to cover up his mistake instead of apologizing.
About the Surgery
According to court documents filed in Connecticut Superior Court, the 60-year-old woman had needed surgery to remove her eighth rib because of a precancerous lesion. This rib had reportedly been marked with metal coils and dye to ensure a successful surgery. Unfortunately, the woman’s seventh rib was removed instead and, instead of performing an X-ray immediately after surgery or contacting the patient to apologize when the mistake was discovered, the woman allegedly had to visit the hospital herself when she continued to experience pain.
Pharmacist Negligence and Liability - Not Always a Cut and Dry Matter
 While a pharmacist’s ability to cause harm is not limited to the medications they do or do not dispense, error can have severe consequences for patients. Take, for example, that a pharmacist dispenses the wrong drug; their patient could be at risk for any number of adverse events, including an allergic reaction, a bad drug interaction (when one drug adversely interacts with another drug), health complications, and even death. Common sense says the pharmacists should be held liable in this situation. Unfortunately, this is not always the case.
While a pharmacist’s ability to cause harm is not limited to the medications they do or do not dispense, error can have severe consequences for patients. Take, for example, that a pharmacist dispenses the wrong drug; their patient could be at risk for any number of adverse events, including an allergic reaction, a bad drug interaction (when one drug adversely interacts with another drug), health complications, and even death. Common sense says the pharmacists should be held liable in this situation. Unfortunately, this is not always the case.
Common Mistakes Made by Pharmacists
Based on an analysis conducted by the Healthcare Providers Service Organization (HPSO), wrong drug dispersion and wrong dose calculation accounted for the majority of the mistakes made by pharmacists over the course of 10 years – 75.3 percent combined (43.8 percent and 31.5 percent, respectively).
Cancer Misdiagnosis and Delays Among Most Common Medical Mistakes
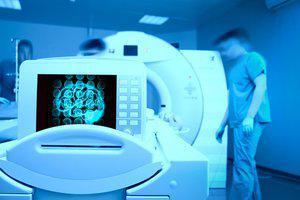 One in 20 adults in the United States (approximately 12 million people) are misdiagnosed by their doctors each and every year. At least half of those people could suffer from serious repercussions. For instance, a Journal of American Medical Association published study found that around 20 percent of all medical errors each year involve delayed cancer diagnosis.
One in 20 adults in the United States (approximately 12 million people) are misdiagnosed by their doctors each and every year. At least half of those people could suffer from serious repercussions. For instance, a Journal of American Medical Association published study found that around 20 percent of all medical errors each year involve delayed cancer diagnosis.
Cancers Commonly Misdiagnosed
According to the previously mentioned study, the most common delayed cancer diagnoses are lung, breast, and colorectal cancers; in fact, they make up about 10 percent of all medical errors. The remaining 10 percent are delayed diagnoses of all other cancers. Examples include ovarian cancers, which a NHS survey found an average diagnostic delay of about 90.3 days; non-Hodgkin’s lymphoma (delayed by an average of 102.8 days); and prostate cancer (average delay of 148.5 days).
Norovirus Deemed as Cause of Michigan State University’s Kellogg Center Outbreak
 Norovirus, an extremely contagious virus, is generally caused by poor hygiene and then spread through food or drink sources. In fact, according to the Centers for Disease Control and Prevention (CDC), about 50 percent of the approximately two million cases each year are contracted through food. This and other possible factors are thought to be responsible for the recent outbreak at Michigan State University’s Kellogg Center.
Norovirus, an extremely contagious virus, is generally caused by poor hygiene and then spread through food or drink sources. In fact, according to the Centers for Disease Control and Prevention (CDC), about 50 percent of the approximately two million cases each year are contracted through food. This and other possible factors are thought to be responsible for the recent outbreak at Michigan State University’s Kellogg Center.
Norovirus Illness
Anyone who is diagnosed with norovirus (or suspects they may have it) should be extremely careful to practice good hygiene and self-isolate whenever possible, even after the symptoms of nausea, diarrhea, vomiting, and stomach pains disappear. This is because, even though no symptoms may be present, norovirus continues to remain in the stool for up to two weeks, creating a risk for self-re-exposure and continued spreading of the virus before, during, and after the actual symptoms appear or disappear.
Preventable Hospital Mistakes Cause Nearly Half a Million Deaths Each Year

Most patients check into a hospital expecting to get better. Sadly, this is not always the case; doctors, surgeons, nurses, anesthesiologists, and other healthcare professionals sometimes make critical mistakes that end up doing more harm than good. Even more disturbing is that, according to recent data, the prevalence of these medical errors has increased over the years at an alarming rate.
Medical Mistakes: Then and Now
It was 1999 when the Institute of Medicine (IOM) published their report, “To Err is Human.” A proverbial bombshell for the medical community, the report claimed that as many as 98,000 people died each year from preventable mistakes made by hospital personnel. Many disputed those figures, saying they were largely exaggerated, but it is now one of the most widely used and quoted research documents on medical errors.
A 2010 statement from the Office of Inspector General for Health, which claimed that bad hospital care contributed to the deaths of 180,000 Medicare patients alone in just a short year, hinted that the problem was growing. Then came the recently published Journal of Patient Safety study, which found that the figures have more than doubled since 1999.
The Most Common Medical Malpractice Errors Made by Doctors (Even the Good Ones)
 According to a recent study, medical malpractice is the third leading cause of death in the United States. Many can be attributed to hospital errors, which can make them immediate and especially critical. However, medical errors with fatal or life-altering consequences do not just occur in hospitals; they can happen in doctor’s offices and clinics as well. Wherever the error happens, the mistakes are often the same, and even the best of doctors can make them.
According to a recent study, medical malpractice is the third leading cause of death in the United States. Many can be attributed to hospital errors, which can make them immediate and especially critical. However, medical errors with fatal or life-altering consequences do not just occur in hospitals; they can happen in doctor’s offices and clinics as well. Wherever the error happens, the mistakes are often the same, and even the best of doctors can make them.
Misdiagnosis
Of all the medical mistakes, misdiagnosis is, by far, the most common. In fact, according to research studies, some 15 percent of conditions are initially misdiagnosed, with urinary tract infections, cancer, congestive heart failure, and acute renal failure being the most common. And, based on a survey from Consumer Reports, these misdiagnoses occur twice as often in doctor’s offices than in hospitals.
Baxter IV Solutions Recalled for Potential Presence of Particulate Matter
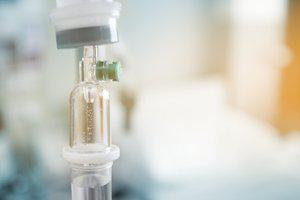 Intravenous (IV) solutions are intended to hydrate or rehydrate patients while under the care of a physician, surgeon, or other applicable healthcare professional. Administration of the solution is handled by licensed professionals, and the patient has no say or knowledge regarding any potential adverse events from a contaminated bag. This makes the recent recall of Baxter IV solutions highly concerning for anyone that has recently visited the hospital, undergone surgery, or otherwise received IV solutions.
Intravenous (IV) solutions are intended to hydrate or rehydrate patients while under the care of a physician, surgeon, or other applicable healthcare professional. Administration of the solution is handled by licensed professionals, and the patient has no say or knowledge regarding any potential adverse events from a contaminated bag. This makes the recent recall of Baxter IV solutions highly concerning for anyone that has recently visited the hospital, undergone surgery, or otherwise received IV solutions.
About the Recall
Comprised of water and electrolytes, the IV solutions were distributed to hospitals and other end users throughout the United States. A customer complaint led to the identification of particulate matter, which was later determined to be an insect. Baxter International Inc. voluntarily recalled all affected lots of the IV solution, but no one knows how many were administered to patients.
Male Enhancement Supplement Recalled Over Undeclared Drug Ingredient
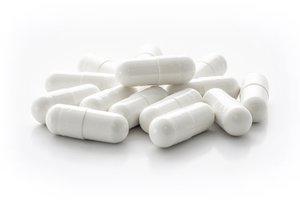 Consumers trust that the items they find on a store shelf are safe, but this is not always the case. A widespread recall of several male enhancement dietary supplements, all marketed and sold by R Thomas Marketing LLC, highlights the risks and dangers of this all too common issue. The voluntary recall of this dangerous and defective drug has not come too late for some.
Consumers trust that the items they find on a store shelf are safe, but this is not always the case. A widespread recall of several male enhancement dietary supplements, all marketed and sold by R Thomas Marketing LLC, highlights the risks and dangers of this all too common issue. The voluntary recall of this dangerous and defective drug has not come too late for some.
About the Recall
Sold and marketed as male enhancement drugs, the tainted dietary supplements (Black Ant, Herb Viagra, Real Skill, Street Overlord, Weekend Prince, and African Black Ant) all contain undisclosed sildenafil, a PDE-5 inhibitor. Although this is the same FDA-approved ingredient found in popular erectile dysfunction drug, Viagra, its lack of disclosure and the potential side effects of the drug (including the potential for bad drug interactions) put users at risk.
Study Says Physicians in Training Can Work Longer Hours
For many years physicians in training, called residents, worked brutally long shifts, barely sleeping over the course of days. As the workhorses of medical care in hospitals, this justifiably led to concerns over errors due to the dangerous combination of inexperience and sleep deprivation. This resulted in rule changes limiting residents to no more than 28 straight hours at the hospital, and 14 hours off after working a 24 hour shift. However, a study in this week’s New England Journal of Medicine has concluded that the reduced resident hours have not impacted patient safety, and is therefore recommending returning to the brutally long shifts of the past. Groups such as the American Medical Student Association are opposing such a rollback, pointing to the “overwhelming” evidence of the dangers of sleep deprivation. In the middle of all of this are hospital patients who expect – and pay for – medical professionals to be at their best.

 312-605-8800
312-605-8800




 312-605-8808
312-605-8808